The latest on liposomes
By Rebecca Guenard
January 2021
- The courier capability of liposomes is being fine-tuned for drug delivery, while researchers continue to imagine new applications.
- Supplement makers are touting the potential benefit of liposomes for increasing the circulation time of vitamins in the blood.
- Researchers have developed a liposome that is capable of promoting cell attachment and growth by delivering an extracellular matrix to cells.
- Liposomes could eventually lead to artificial cells that reveal the origin of life.
Since 1961, when images from an electron microscope first revealed the bilayer lipid structure of cell membranes, researchers have been intrigued by their potential. The scientist who made the discovery, Alec Douglas Bangham, at Babraham Institute in Cambridge, Massachusetts, USA, observed that, like a microscopic parcel, the closed structure released its contents when exposed to a detergent. He called the structures “liposomes”.
The lipid bilayer of liposomes creates a unique vessel that’s utility was immediately recognized as a means for stealthily delivering drugs to sites of disease in the human body. The hydrophobic membrane encapsulates an aqueous core where hydrophilic molecules can be contained. Liposomes can also encapsulate molecules that do not dissolve in water. Hydrophobic molecules trapped inside them will cling to the interior bilayer walls. In fact, the physical properties of liposomes allow for a diversity of compounds and pH ranges to reside within the structure without detection by the body’s immune system.
“Lipids are biologically friendly molecules,” says Kwanwoo Shin, professor at Sogang University in Soul, Korea. “They are very stable in our biological systems.”
In the decades since their discovery, pharmaceutical companies have developed a range of clinically approved liposome-based medicines. They are ideal for drugs with poor pharmacokinetics, limited bioavailability, or a high degree of toxicity. As the field of nano-medicine grows, the biocompatibility of liposomes and lipid nanoparticles will continue to make them a valuable asset for drug delivery.
In fact, lipid nanoparticles are a critical part of the COVID-19 vaccines being produced by Pfizer and Moderna. Both manufacturers use lipids to shield delicate mRNA long enough for it to be delivered to cells. There, the mRNA signals the cell to produce a coronavirus protein that induces a mild immune response, prepping the body for future COVID-19 exposure. A Moderna representative has stated that its unique combination of four different lipids sufficiently protect mRNA from degrading, thus requiring a lower storage temperature than the Pfizer vaccine (https://tinyurl.com/covidmRNAvaccines).
Along with their established role in pharmaceuticals, these lipid-based compounds have enhanced the effectiveness of products for the beauty and supplement industries. And researchers are getting more innovative about liposome applications, even using them to make artificial cells. Here are some of the latest commercial and research applications.
A nanomedicine
“Liposomes prolong circulation of a drug in the body, breaking down without being expelled through the kidneys, for a slow release of the active ingredient,” says Claudia Zylberberg, CEO at Akron Biotech, in Boca Raton, Florida, USA. The company provides products and services to biopharmaceutical companies (https://www.akronbiotech.com). The US Food and Drug Administration (FDA) approved liposomes as the first nanoscale drug in 1995. Since then, development has centered on delivering a target compound to a specific location, within a specific time, and at a desired permeation rate. Researchers alter the composition of phospholipids in the bilayer to tailor the drug release profile for specific applications.
Early on, interactions with circulating blood proteins destabilized liposomes, and they were cleared from the body shortly after injection. The drug carriers became more effective after they were coated with inert hydrophilic polymers, such as polyethylene glycol (PEG). The improvement increased circulation time and, thus, bioavailability, earning these modified versions the name “stealth liposomes”.
Coating liposomes has led to their improved effectiveness in targeting specific treatment areas. Ligands attached to the stealth liposome shell home in on unique disease environments and selectively deliver a drug. Cancer therapies center on overexpressed cell receptors that occur with malignancy. Connecting ligands of certain enzymes, folic acid, or monoclonal antibodies to the exterior of the liposomes is like providing a key that can access cancer cells. Once the liposomes have gained access, they unleash their cancer-killing cargo.
“It is also possible to have them break down in a certain environment,” says Zylberberg. “Like in a capillary where there is a lot of oxygen and CO2 exchange actively changing the local environment to have a lower pH.”
Customized liposome coatings have resulted in successful clinical trials for liposome-based drugs to treat fungal infections, meningitis, hepatitis, as well as a variety of cancers. In clinical studies, the pharmacokinetics and biodistribution surpass traditional treatments while minimizing toxicity.
Zylberberg says she will not be surprised if the success of liposomes as delivery vehicles that can be modified for cell penetration will lead to their application in more and more commercialized products.
Encapsulating supplements
Many of the vitamins sold as supplements do not produce as much benefit as they could because of a lack of bioavailability. The majority are not absorbed by the body. They are broken down during digestion and expelled.
Some supplement makers have caught on to the potential benefit of liposomes for increasing the circulation time of vitamins in the blood. A company called SOMEGA, in Cork, Ireland, has just launched a liposome-coated vitamin C supplement. One of the company’s co-founders claim the new technology improves absorption by enhancing delivery of vitamin C to the cells (https://tinyurl.com/supplementswithliposomes).
A company in Rehoboth Beach, Delaware, USA, is making a similar claim. Manna is promoting a liposomal curcumin that they say enhances powdered turmeric’s pain-reducing and anti-inflammation capabilities (https://curcumin.mannaboost.com). The company cites scientific studies that support their claims. In fact, recently published research on small groups of participants show an increase in bioavailability with liposome-encapsulated supplements.
Researchers compared intravenous, oral, and liposomal vitamin C supplements (Fig. 1) and found that encapsulating the vitamin resulted in a higher concentration in the blood when taken orally than occurred with non-encapsulated supplements (https://doi.org/10.4137/NMI.S39764). Typically, vitamin C must be administered intravenously to achieve a significant amount in blood plasma. Oral doses of the supplement do not make it through the renal system without decomposing. However, the longer vitamins are in the blood stream, the greater the chance they will be absorbed into cells and counter the effects of oxidative stress. The conclusion of liposomal vitamin studies is that these nanoparticles provide users with the critical benefit of a longer duration in the blood stream (https://doi.org/10.1080/08982104.2019.1630642).

Beauty and healing
The beauty industry has also taken advantage of liposomes as a means for delivering molecules to cells. The market has a myriad of anti-aging products encapsulated in liposomes to improve effectiveness.
Shin says it is not enough to coat an anti-aging ingredient. The synthesis needs to be strategic. The properties of the liposome and its contents must be planned properly to achieve the desired outcomes for a specific application, he adds. For precisely controlled delivery to a target, you need to make the exact sized nanoparticle containing the exact compound with the exact molecular structure.
“If the particle size is much smaller than the cell size of human skin, then the particles start to penetrate the cell directly,” Shin explains. “If the size is bigger, then the cell naturally repels it.” He is currently collaborating with Harvard researchers on a new liposome delivery system for collagen.
The problem is collagen is a huge molecule, according to Shin. “Sometimes people drink it or apply it directly, but it is too big to penetrate inside a cell.” Shin and his collaborators have developed liposomes containing tropocollagen molecules, smaller collagen subunits that link together to make up a full collagen molecule. They are small enough to penetrate deep into the skin and enter cells. An external stimulation source, like the light from an LED mask, dismantles the liposomes, spilling its contents, which cells then use to build collagen fiber in situ. Skin cells excrete the collagen into intercellular space, replacing what is lost naturally with age.
Shin says this liposomal collagen product has been successfully tested on animals. The group hopes to commercialize it next year. Concurrently, they are applying their process for developing this product to create a treatment for healing wounds.
“Healing is a natural process, but to facilitate it we are adding liposomes with extra cellular matrix proteins,” Shin says.
Fibronectin, laminin, and elastin are some of the proteins that compose the body’s connective tissue. When an injury occurs, they remodel the skin and formulate scar tissue.
Shin and his team have combined these proteins with liposomes and found that the additional cellular matrix proteins alone accelerate healing. “Even without drugs we can make the cells more active, more fast moving so they can heal much faster,” he says.
This is particularly important for burn victims. After a burn, skin scars quicker than cells can rebuild the original shape, permanently changing its structure. But if you activate the cells with liposomes containing the necessary proteins, then you can entice it to rebuild the skin before scarring occurs, Shin says. Perhaps all bandages could be infused with this treatment to improve wound healing.
Artificial cells
Shin views the applications he described as a means to an end. What he is most interested in studying is the fundamental mechanism for cellular function. To do that, he uses liposomes to recreate the organelles and membranes that comprise a living cell.
Shin explains that a classic liposome study focuses on optimizing the shape of the lipid bilayer for a specific target. His research group is working with shape as well as function, so the liposome behaves like an actual cell.
“This is really complex, but we went through one function at a time. Then we combined them incrementally,” he says. “The whole architecture is just made of lipids and proteins.”
Building a cell from the ground up inevitably involves the challenge of having to duplicate the complex metabolic reactions that cells need to operate. Shin’s team addressed the challenge by using light, in a type of photosynthesis, to initiate cell processing. They embedded proteins and enzymes in a lipid membrane which produced adenosine triphosphate (ATP) when activated. Switching the light to a different wavelength stops the reaction. ATP provides the energy necessary for the cells to generate actin, a protein that forms filaments of muscle cells. The experiment, published in Nature Biotechnology (https://doi.org/10.1038/nbt.4140), proved that liposomes could be used to make a functioning artificial cell (Fig. 2).
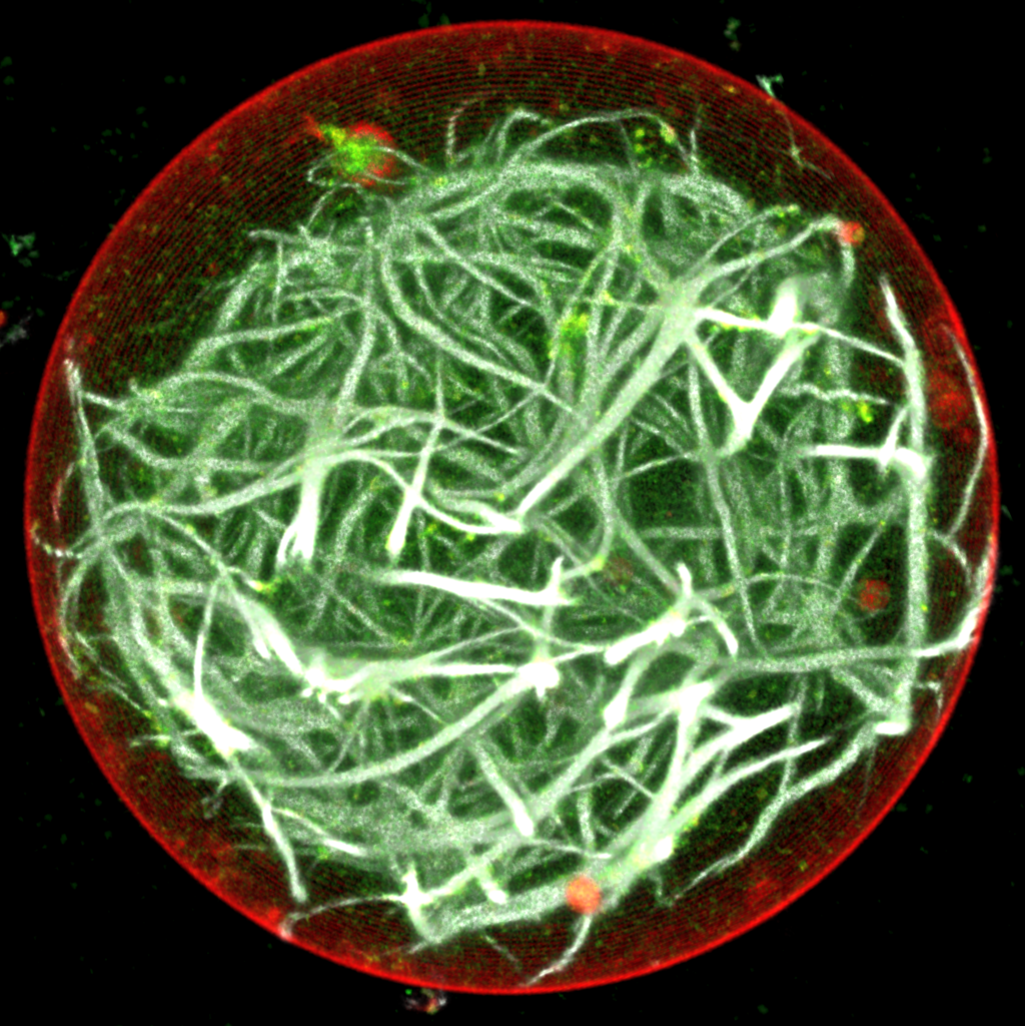
Shin plans to continue his international collaboration with the Harvard researchers in pursuit of creating fully operational artificial cells. He says that these types of cells could be used to identify how a disease manifests and, ultimately, how to cure or eliminate that disease. Primarily, he is curious about life.
“There was a protein; there was a lipid; there were many other things,” says Shin. “Somehow they assembled to become bacteria, to become viruses, to become mammalian cells.” In the future, he wants to perform fundamental studies to understand how multi-celled organisms developed. “We could use artificial cells to learn how human life originated,” says Shin.
The human body is teeming with lipids. Liposomal cloaks take advantage of that fact and allow researchers to sneak crucial drug treatments past the body’s immune system. Over the decades, they have gotten better at disguising drugs so that nefarious cells do not suspect the threat that lies inside. It is remarkable what scientists can do with a group of amphiphilic molecules. They may even someday provide the answer for the origins of life on Earth.
Rebecca Guenard is the associate editor of INFORM at AOCS. She can be contacted at rebecca.guenard@aocs.org.
Information
Tumor repolarization by an advanced liposomal drug delivery system provides a potent new approach for chemo-immunotherapy, Ringgaard, L., et al., Sci. Adv. 6: 36, 2020.
Photosynthetic artificial organelles sustain and control ATP-dependent reactions in a protocellular system, Lee, K.Y., et al., Nat Biotechnol. 36: 530–535, 2018.
Pharmaceutical liposomal drug delivery: a review of new delivery systems and a look at the regulatory landscape, Zylberberg, C. and S. Matosevic, Drug Delivery 23: 9, 2016.
Liposomal-encapsulated ascorbic acid: influence on vitamin C bioavailability and capacity to protect against ischemia–reperfusion injury, Davis, J.L., Nutrition and Metabolic Insights, January 2016.


