The brain accounts for about 2% of our body weight, but consumes nearly 25% of our food’s energy. It is hungry for a healthy diet. The food we eat affects how we think, how we feel, and how we view the world. A poor diet has been linked to irritability, cognition loss, and an increase in stress, anxiety, and confusion. While the Mediterranean and MIND (Mediterranean-DASH Intervention for Neurodegenerative Delay) diets have been associated with longer lifespans and lower risk of cardiovascular disease and diabetes.

- Are there foods that will stave off cognitive decline and neurodegenerative disease, or even reduce depression symptoms? According to the latest research, the answer is yes.
- Scientists are using model cell lines that mimic Parkinson’s and Alzheimer’s to determine the mechanisms for phospholipid involvement in these diseases and how diet can protect the compounds from oxidation.
- At the same time, large consortia studies show that DHA and EPA intake correlate with better cognitive function and improved mood.
Both diets incorporate whole ingredients rich in fruits, vegetables, and whole grains. Both add healthy fats from olive oil, avocado, and nuts. The diets also favor omega-3-rich plants and seafood while limiting the intake of processed foods and red meat.
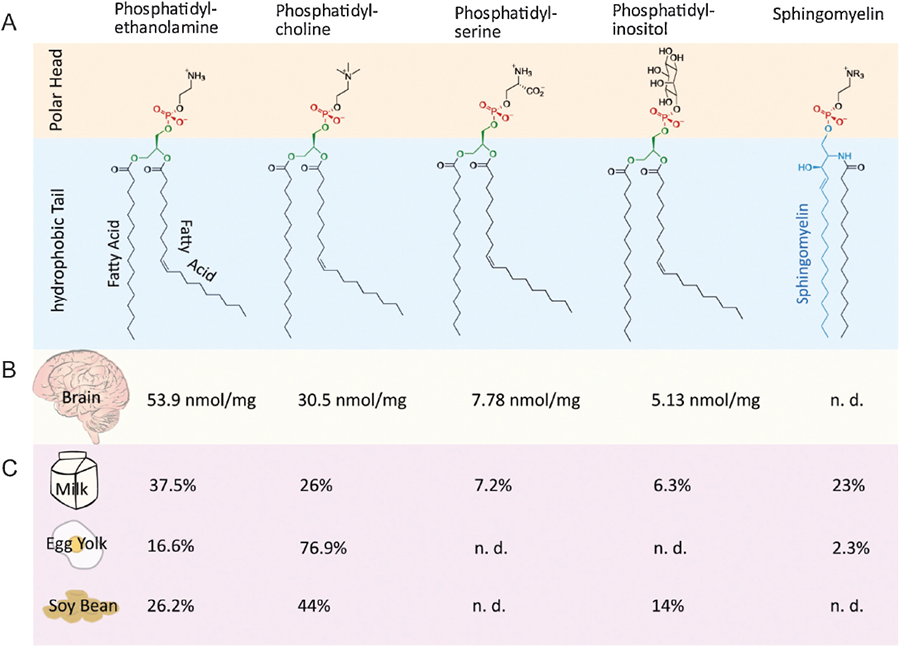
FIG. 1. Different classes of phospholipids. A: structure of the different phospholipids. B: Brain distribution of phospholipids per mg of tissue. C: Distribution of phospholipids in the main dietary sources, expressed in % of total phospholipids. Source: Schverer, M., et al., NeuBioRev, 111, 183, 2020.
"The Mediterranean diet has lots of components that we think are beneficial in terms of mechanisms to improve mental health," said Jessica Bayes, research fellow at Southern Cross University in Lismore, Australia.
The importance of these diets becomes particularly clear as people are living longer. According to a report by the United Nations, Department of Economic and Social Affairs, the global population over 60 years old has doubled in the last 30 years and is expected to double again by 2050 (https://tinyurl.com/yxjexbh6).
Cognitive function peaks around middle age then begins to decline, even in healthy people. Oxidative stress, chronic inflammation, and vascular changes can impair synaptic activity at a time when the aging brain also begins to lose neurons. These factors leave a person vulnerable to dementia as they age. By 2030, the World Health Organization estimates 70 million people will experience dementia worldwide (https://tinyurl.com/ycybmjkn).
Decades of research has been dedicated to understanding the relationship between dietary patterns, dementia, and neurodegenerative disease. Scientists have found that maintaining healthy cognitive and metabolic functions can be assisted by being selective with daily dietary consumption. Foods and nutrients that may prevent cognitive decline, including fruits, vegetables, fish, monounsaturated fats, polyunsaturated fats, and antioxidants.
PHOSPHOLIPID COMPOSITION
Glycerophospholipids (GPL) are key components of cell membranes. They are the major source of long-chain polyunsaturated fatty acids (PUFA) and the reservoir of signaling molecules. As the brain ages, lipidomic studies show that phospholipid populations in the cerebellum undergo major change.
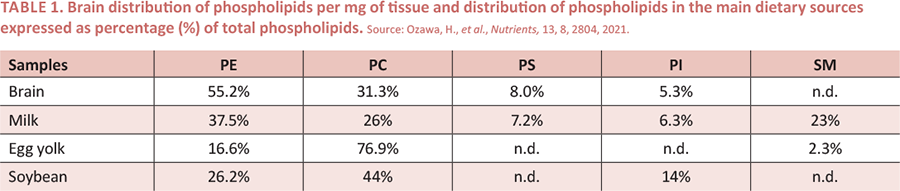
Glycerophospholipids in cell membranes mainly include phosphatidylcholine (PC), phosphatidylethanolamine (PE), phosphatidylserine (PS), and phosphatidylinositol (PI) (Fig.1). These lipids and their metabolites participate in blood brain barrier function, the inflammation processes, and membrane remodeling, among other functions. Therefore, they have been highlighted in terms of their impact on cognition, with PC and PS being the most widely studied. Soybean and animal products, like meat and eggs, are prominent dietary sources of these polar lipids (Table 1).
Both human and animal studies have confirmed that phospholipid supplements can improve cognitive decline resulting from stress and aging. One preclinical study used a diet supplemented with complex milk lipid concentrate rich in phospholipids, and another used oral administration of PS isolated from krill or soy (https://doi.org/10.1016/j.pnpbp.2010.05.031). The PS groups in these studies showed marked improvement in both behavior and cognition when compared to the placebo group. Since phospholipids are essential for brain function, consuming food containing these compounds has a significant impact on reducing cognitive decline related to aging.
In 1988, scientists discovered that, similar to lipid oxidation in food, membrane phospholipids in the human body oxidize into phospholipid hydroperoxides (doi: 10.1093/oxfordjournals.jbchem.a122339). Since then, many researchers have studied how consuming flavonoids and other polyphenols affect cognitive performance. While the results of these studies are somewhat mixed, a contingent of studies do show measurable cognitive improvement in older adults.
Scientists are working out a more detailed picture of phospholipid reactions in the brain by conducting in vitro measurements with model cell lines. Most studies are using the cells as a stand-in for pathologies, like Parkinson’s and Alzheimer’s. However, the results associated with these studies indicate certain dietary compounds reduce oxidative stress, along with how to avoid inflammation-induced cell and tissue injuries.
While we await further understanding of the cellular-level phospholipid mechanisms that occur based on specific dietary components, several long-term studies reveal the importance the types of food we consume have on brain health, in particular, omega-3 fatty acids.
DHA KEEPS YOU SHARP
Dementia is a progressive disease that affects cognition—such as, working memory and processing speed—and can hinder the ability to perform daily tasks. The path to contracting dementia is paved by diet, genetics, and social context decades before the onset of symptoms. To mitigate the potential consequences, doctors encourage people to adopt protective habits, including physical activity, weight management, tobacco cessation, and eating a healthy diet.
During the 2017 Health Retirement Study, researchers evaluated more than 5,000 older adults with an average age of 68 years who followed either the MIND or Mediterranean diet (https://doi.org/10.1111/jgs.14922). They assessed outcomes using MedDiet score (0 to 55) and MIND diet score (0 to 15), each based on frequency of eating the 11 or 15 food groups of the respective diets. After assessing the cognitive performance of the older adults, the researchers found the diets bestowed neuroprotective benefits. In fact, people following these diets closely have a 30 to 35% lower risk of becoming cognitively impaired.
In the years that followed, more studies suggested that DHA, an important component of the Mediterranean diet, mitigates many of the factors that contribute to dementia and Alzheimer’s disease.
To investigate this claim, William Harris, president and founder of the Fatty Acid Research Institute in Sioux Falls, South Dakota, USA, and his team evaluated data collected from the Framingham Heart Study (https://doi.org/10.3390/nu14122408). The study began in 1948 and continues to follow a representative group of healthy people living in the town of Framingham, Massachusetts. Participants in the study are contacted every four years to obtain health outcomes, with a particular focus on cardiovascular health. Harris and his team used this dataset to examine the connection between blood DHA levels and cognitive ability.
Most nutrition studies are hindered by self-reported diet information. To circumvent this complication, Harris and his colleagues chose to focus on the level of DHA in the bloodstream. Red blood cells typically remains in the body for 120 days, so DHA concentration offers a reliable marker of omega-3 intake.
Of the original 5,124 participants enrolled in the Framingham study, 3,021 attended the eighth health cycle between 2005 and 2008. Harris and his team narrowed the group further using exclusion criteria. Participants that carried the APOE2 allele, which has a protective effect against cognitive decline, were removed from the analysis. Participants younger than 65 or who already had dementia were also removed. The group analyzed for this study consisted of 1,490 individuals. Blood DHA was measured from baseline samples, and Harris and his team followed this smaller group for the next 14 years.
The research team found that DHA was a positive marker to support cardiovascular and cognitive health. Participants with higher levels of DHA in their blood delayed the onset of Alzheimer’s disease by 4.7 years and all-cause dementia by four years. Participants who carried the APOE4 allele, which is a marker of increased risk for Alzheimer’s disease, benefited by having more DHA in their diet. Harris and his team also evaluated the protective status of the omega-index (EPA + DHA) compared to DHA alone but did not see any added benefit of higher EPA levels from the study.
EPA LIGHTENS THE MOOD
A recent study published in the American Journal of Preventive Medicine found adolescents and young adults (age 12 to 25) experienced higher levels (17%) of depression (https://doi.org/10.1016/j.amepre.2022.05.014). Beyond the age of 35, the prevalence of depression stabilizes and remains low, but cognition begins to decline, with the most pronounced effects appearing decades later (https://doi.org/10.1016/j.neurobiolaging.2008.09.023).
Depression is a mood disorder of the brain that affects about 350 million people around the world. It manifests as feelings of irritability, fatigue, anxiety, and the loss of interest and joy in life. The standard treatments for depression include behavioral therapy and antidepressant medications, but 30% of people with moderate to severe symptoms do not respond to drug therapy. Nutrition offers another way to manage this mental disorder.
People with depression are often encouraged to eat a healthful diet. Both the Mediterranean and MIND diets reduce inflammation, which may play a role in the activation of neurotransmitters and strengthen brain cells and brain plasticity.
"EPA is one form of the omega-3s that are an important component of this diet, which requires a high intake of fish and seafood," said Bayes.
Bayes led the team that conducted the AMMEND clinical trial, which sought to understand the role of nutrition on mental health (https://doi.org/10.1093/ajcn/nqac106). This study enrolled 72 men (18 to 25 years) who had been diagnosed with moderate to severe major depressive disorder but did not respond to common anti-depressant medications. Participants were randomly assigned into one of two groups.
Half the men received nutritional counseling from a clinical nutritionist and learned how to add components of the Mediterranean diet into their daily meal prep. The remaining participants were enrolled in befriending support sessions that involved discussion of neutral topics, like sports or hobbies. At the end of 12 weeks, the participants in the nutritional intervention group showed greater improvement over the control group in their symptoms and quality-of-life measures, like concentration, sleep, and energy.
The Mediterranean diet was a more effective intervention in the AMMEND study and could inform new approaches to help people manage their depression symptoms, but the study did not focus on a direct causal mechanism to explain how EPA might affect depressive symptoms. Depression is believed to arise through the combination of biology, social factors, and psychological factors.
Bayes points to biological pathways addressed in previous studies that the fatty acid could touch, like inflammation and oxidative stress, but other factors, including mitochondrial dysfunction, epigenetics, the gut microbiome, tryptophan–kynurenine metabolism, the hypothalamic-pituitary axis, neurogenesis, and brain-derived neurotrophic factor, could also play a role. The mechanistic role of EPA in mitigating depression is open for future studies. Beyond the fatty acid mechanics, the mere focus on self-care, learning a new skill, focusing on healthful foods, and pairing food and social interactions can be very therapeutic.
Bayes acknowledges that not everyone has the tastebuds or finances to eat fish all of the time. She encourages people to focus on purchasing high-quality foods at the grocery store and begin the process of slowly adding new foods into their diet. In the long run, the small changes can add up to have a big health effect.
"We know there is a psychological and social aspect of food," said Bayes. "Choosing healthier food boosts self-esteem in addition to the other beneficial aspects."
The daily recommended intake of EPA and DHA is equivalent to 3 ounces of fish, like salmon, sardines, albacore tuna, or herring (about the size of a deck of playing cards) three to five times a week. Despite this widely held recommendation, a recent study found that only 24% of the world’s adult population meets the required DHA recommendation (https://doi.org/10.1002/fsn3.2299). EPA and DHA supplements could address this need, but supplements vary in dosage and quality.
New formulation techniques could extend the shelf life and efficacy of DHA and EPA (https://doi.org/10.1002/fsn3.2299). Microencapsulating these compounds into an emulsion could reduce oxidation and mask the strong odor. Particularly since, emulsified fish oil dissolves along the digestive tract for faster, more efficient nutrient absorption compared to fish oil encased in gelatin capsules.
In 2021, the cost of healthcare for people with Alzheimer’s disease reached $355 billion, raising the urgency to find new therapies that delay or minimize the onset of Alzheimer’s disease and dementia.
"DHA seems to work well to preserve brain health into older age," said Harris. "We are trying to forestall the development of dementia and want to understand the mechanism by which it acts so that we can possibly design better therapies."
About the Author
Stacy Kish is a science writer for INFORM and other media outlets. She can be contacted at earthspin.science@gmail.com